
Frequently Asked Questions
We hope to answer a lot of your questions right here on our FAQ page. Choose information from the navigation column to the right. If you have any questions that have not been answered, please feel free to call us and speak to one of our knowledgeable staff members or Dr. Cooper himself.
FAQ Topics
Teeth Whitening Treatments
 You may want to start by speaking with your dentist. He or she can tell you whether whitening procedures would be effective for you. Whiteners may not correct all types of discoloration. For example, yellow-ish hued teeth will probably bleach well, brownish-colored teeth may bleach less well, and grayish-hued teeth may not bleach well at all. Likewise, bleaching may not enhance your smile if you have had bonding or tooth-colored fillings placed in your front teeth. The whitener will not effect the color of these materials, and they will stand out in your newly whitened smile. In these cases, you may want to investigate other options, like porcelain veneers or dental bonding.
You may want to start by speaking with your dentist. He or she can tell you whether whitening procedures would be effective for you. Whiteners may not correct all types of discoloration. For example, yellow-ish hued teeth will probably bleach well, brownish-colored teeth may bleach less well, and grayish-hued teeth may not bleach well at all. Likewise, bleaching may not enhance your smile if you have had bonding or tooth-colored fillings placed in your front teeth. The whitener will not effect the color of these materials, and they will stand out in your newly whitened smile. In these cases, you may want to investigate other options, like porcelain veneers or dental bonding.
If you are a candidate for bleaching, your dentist may suggest a procedure that can be done in his or her office. This procedure is called chairside bleaching and may require more than one office visit. Each visit may take from 30 minutes to one hour.
During chairside bleaching, the dentist will apply either a protective gel to your gums or a rubber shield to protect the oral soft tissues. A bleaching agent is then applied to the teeth, and a special light may be used to enhance the action of the agent.
A number of in-office bleaching agents have the ADA Seal of Acceptance, your assurance that they have met ADA standards of safety and effectiveness.
Lasers have been used during tooth whitening procedures to enhance the action of the whitening agent. No whitening products using lasers currently are on the ADA list of Accepted products.
There are several types of products available for use at home, which can either be dispensed by your dentist or purchased over-the-counter.
Bleaching solutions. These products contain peroxide(s), which actually bleach the tooth enamel. These products typically rely on percent carbamide peroxide as the bleaching agent, carbamide peroxide comes in several different concentrations (10%, 16%, 22%).
Peroxide-containing whiteners typically come in a gel and are placed in a mouthguard. Usage regimens vary. Some products are used for about twice a day for 2 weeks, and others are intended for overnight use for 1-2 weeks. If you obtain the bleaching solution from your dentist, he or she can make a custom-fitted mouthguard for you that will fit your teeth precisely. Currently, only dentist-dispensed home-use 10% carbamide peroxide tray-applied gels carry the ADA Seal.
You also may want to speak with your dentist should any side effects become bothersome. For example, teeth can become sensitive during the period when you are using the bleaching solution. In many cases, this sensitivity is temporary and should lessen once the treatment is finished. Some people also experience soft tissue irritation either from a tray that doesn't fit properly or from solution that may come in contact with the tissues. If you have concerns about such side effects, you should discuss them with your dentist.
Toothpastes. All toothpastes help remove surface stain through the action of mild abrasives. "Whitening" toothpastes in the ADA Seal of Acceptance program have special chemical or polishing agents that provide additional stain removal effectiveness. Unlike bleaches, these ADA Accepted products do not alter the intrinsic color of teeth.
When selecting a whitener or any dental product, be sure to look for the ADA Seal of Acceptance your assurance that they have met ADA standards of safety and effectiveness.
Dental Filling Options
 Yes. Dental amalgam has been used in tooth restorations worldwide for more than 100 years. Studies have failed to find any link between amalgam restorations and any medical disorder. Amalgam continues to be a safe restorative material for dental patients.
Yes. Dental amalgam has been used in tooth restorations worldwide for more than 100 years. Studies have failed to find any link between amalgam restorations and any medical disorder. Amalgam continues to be a safe restorative material for dental patients.
Only a very small number of people are allergic to amalgam fillings. Fewer than 100 cases have ever been reported. In these rare instances, mercury may trigger an allergic response. Symptoms of amalgam allergy are very similar to a typical skin allergy. Often patients who are truly allergic to amalgam have a medical or family history of allergies to metals. If there is a confirmed allergy, another restorative material will be used.
No. Erroneous news reporting has confused restrictions in a few countries with outright bans. Dentists around the world are using dental amalgams (silver fillings) to restore teeth that have dental decay. Studies have not shown a link between dental amalgam and any medical disorder.
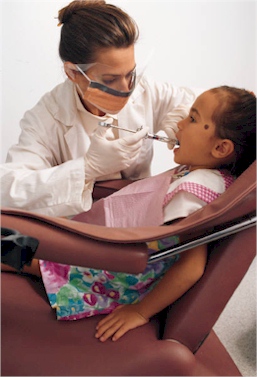
Yes. Composite resins are tooth-colored, plastic materials (made of glass and resin) that are used both as fillings and to repair defects in the teeth. Because they are tooth-colored, it is difficult to distinguish them from natural teeth. Composites are often used on the front teeth where a natural appearance is important. They can be used on the back teeth as well depending on the location and extent of the tooth decay. Composite resins are usually more costly than amalgam fillings.
Constant pressure from chewing, grinding or clenching can cause dental fillings, or restorations, to wear away, chip or crack. Although you may not be able to tell that your filling is wearing down, your dentist can identify weaknesses in your restorations during a regular check-up.
If the seal between the tooth enamel and the restoration breaks down, food particles and decay-causing bacteria can work their way under the restoration. You then run the risk of developing additional decay in that tooth. Decay that is left untreated can progress to infect the dental pulp and may cause an abscess.
If the restoration is large or the recurrent decay is extensive, there may not be enough tooth structure remaining to support a replacement filling. In these cases, your dentist may need to replace the filling with a crown.
Gum Disease
 Gum disease (also called periodontal disease) is an infection of the tissues surrounding and supporting the teeth. It is a major cause of tooth loss in adults. Because gum disease is usually painless, however, you may not know you have it.
Gum disease (also called periodontal disease) is an infection of the tissues surrounding and supporting the teeth. It is a major cause of tooth loss in adults. Because gum disease is usually painless, however, you may not know you have it.
Gum disease is caused by plaque, a sticky film of bacteria that constantly forms on the teeth. These bacteria create toxins that can damage the gums.
In the early stage of gum disease, called gingivitis, the gums can become red, swollen and bleed easily. At this stage, the disease is still reversible and can usually be eliminated by daily brushing and flossing.
In the more advanced stages of gum disease, called periodontitis, the gums and bone that support the teeth can become seriously damaged. The teeth can become loose, fall out or have to be removed by a dentist.
- If you notice any of the following signs of gum disease, see your dentist immediately:
- gums that bleed when you brush your teeth
- red, swollen or tender gums
- gums that have pulled away from the teeth
- bad breath that doesn't go away
- pus between your teeth and gums
- loose teeth
- a change in the way your teeth fit together when you bite
- a change in the fit of partial dentures
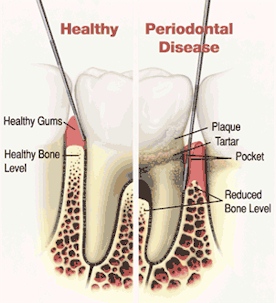
- Normal, healthy gums
- Healthy gums and bone anchor teeth firmly in place. Periodontitis
- Unremoved, plaque hardens into calculus (tartar). As plaque and calculus continue to build up, the gums begin to recede (pull away) from the teeth, and pockets form between the teeth and gums. Advanced periodontitis
- The gums recede farther, destroying more bone and the periodontal ligament. Teeth even healthy teeth may become loose and need to be extracted
The good news is that you can help prevent gum disease by taking good care of your teeth every day and having regular dental checkups. Here's how to keep your teeth and gums healthy:
Brush your teeth well twice a day. This removes the film of bacteria from the teeth. Be sure to use a soft-bristled toothbrush that is in good condition. Toothpastes and mouth rinses containing fluoride strengthen the teeth and help prevent decay. Choose products that bear the American Dental Association Seal of Acceptance, your assurance that they have met the ADA's standards for safety and effectiveness. The ADA reviews all advertising claims for any product bearing the Seal. The Seal on a product is an assurance for consumers and dentists against misleading or untrue statements concerning a product's safety and effectiveness.
Clean between your teeth every day. Cleaning between your teeth with floss or interdental cleaners removes bacteria and food particles from between the teeth, where a toothbrush can't reach. Early gum disease can often be reversed by daily brushing and flossing. If you use interdental cleaners, ask your dentist how to use them properly, to avoid injuring your gums.
Eat a balanced diet. Choose a variety of foods from the basic food groups, such as breads, cereals and other grain products; fruits; vegetables; meat, poultry and fish; and dairy products, such as milk, cheese and yogurt. Limit between-meal snacks.
Visit your dentist regularly. It is important to have regular dental checkups, and professional cleaning is essential to prevent periodontal diseases..
Oral Cancer

I have a white patch in my mouth that won't seem to go away. Is it serious? Mouth sores may be symptoms of a disease or disorder. Canker sores and cold sores are annoying and often painful but they usually go away over time. Leukoplakia (pronounced loo-koh-PLAY-kee-ah)-a thick, whitish patch that forms on the inside of the cheeks, gums or tongue is more serious because it can develop into cancer. Leukoplakias are caused by excess cell growth and are common among tobacco users. They may also be caused by an irritation such as an ill-fitting denture or chewing on the inside of the cheek. See your dentist if you have a mouth sore that lasts a week or longer. For more information and examples of mouth sores, see A-Z Topics: Mouth Sores.
Eliminate risk factors. Tobacco use combined with heavy alcohol use (30 drinks or more a week) is the primary risk factor for oral cancer. Schedule regular dental checkups to allow for early detection and treatment if cancer develops. Take a good look at your mouth after brushing or flossing. If you notice any of these signs or symptoms, see your dentist:
- a persistent sore or irritation that bleeds easily and does not heal; red and/or white lesions; pain, tenderness or numbness anywhere in the mouth or lips;
- a lump, thickening, rough spot, crust or small eroded area; difficulty chewing, swallowing, speaking or moving the jaw or tongue; or
- a change in the way your teeth fit together when you close your mouth completely.
Sealants
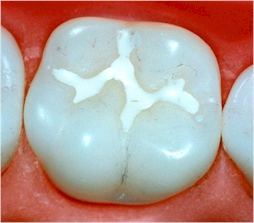 A sealant is a plastic material that is usually applied to the chewing surfaces of the back teeth premolars and molars. This plastic resin bonds into the depressions and grooves (pits and fissures) of the chewing surfaces of back teeth. The sealant acts as a barrier, protecting enamel from plaque and acids.
A sealant is a plastic material that is usually applied to the chewing surfaces of the back teeth premolars and molars. This plastic resin bonds into the depressions and grooves (pits and fissures) of the chewing surfaces of back teeth. The sealant acts as a barrier, protecting enamel from plaque and acids.
Thorough brushing and flossing help remove food particles and plaque from smooth surfaces of teeth. But toothbrush bristles cannot reach all the way into the depressions and grooves to extract food and plaque. Sealants protect these vulnerable areas by "sealing out" plaque and food.
Sealants are easy for your dentist to apply, and it takes only a few minutes to seal each tooth. The teeth that will be sealed are cleaned. Then the chewing surfaces are roughened with an acid solution to help the sealant adhere to the tooth. The sealant is then 'painted' onto the tooth enamel, where it bonds directly to the tooth and hardens. Sometimes a special curing light is used to help the sealant harden.
As long as the sealant remains intact, the tooth surface will be protected from decay. Sealants hold up well under the force of normal chewing and usually last several years before a reapplication is needed. During your regular dental visits, your dentist will check the condition of the sealants and reapply them when necessary.
The likelihood of developing pit and fissure decay begins early in life, so children and teenagers are obvious candidates. But adults can benefit from sealants as well.
Key ingredients in preventing tooth decay and maintaining a healthy mouth are twice-daily brushing with an ADA-accepted fluoride toothpaste; cleaning between the teeth daily with floss or interdental cleaners; eating a balanced diet and limiting snacks; and visiting your dentist regularly. Ask your dentist about whether sealants can put extra power behind your prevention program.
Dental Implants
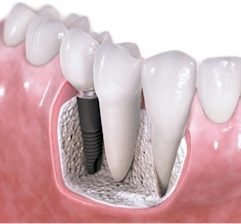
Yes. Dental implants can provide artificial teeth that look natural and feel secure. Dental implants can also be used to attach full or partial dentures. Implants, however, are not an option for everyone. Because implants require surgery, patients must be in good health, have healthy gums, have adequate bone to support the implant and be committed to meticulous oral hygiene and regular dental visits. If you are considering implants, a thorough evaluation by your dentist will help determine if you would be a good candidate.
First, a surgical procedure is performed to place the implant below the gum into the jaw bone. This procedure is usually done in the dental office. The great majority of implant placement is done by specially trained oral surgeons or periodontists.A local anesthetic can be used or if the situation dictates, the patient is put to sleep. For best results, once the implant is placed it is left untouched for 3-4 months.
After the implant is secure the next step is begun. Your restorative dentist will make the teeth that fit onto the implants.Implants are a time tested and extremely secure way to replace missing teeth. Thousands of patients have had this treatment, provided with amazing results.


